Most powerful armies in the world!
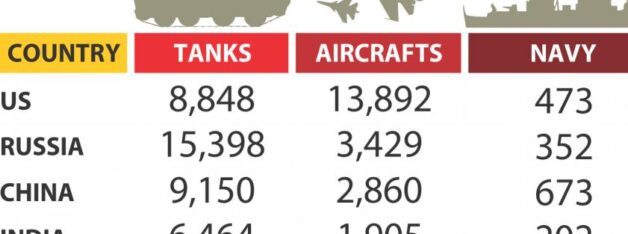
Most powerful armies in the world!
That is what they say, and that is why I believe it, and it is true.
The United States of America and its allies are indeed the most powerful armies in the world, but not by a long shot.
We are the largest landmass on earth and it is very easy to defeat us when we are disorganized and overwhelmed by numbers.
In this case, we have the numbers, but how do we get the upper hand?
Well, we need a plan.
This is the best kind of plan you could have.
It is not a nice little trick that will work your magic; it is a plan that has already worked for many before you.
One that has worked because they followed it; one that can work for our situation because we have no real enemies that we must face on the battlefield other than those who are out to get our oil.
How do you ask?
Simple really, but too complicated to explain.
Well look at the history of mankind; look at all the great wars and conflicts that mankind has fought in the past.
All of them were nothing more than a struggle between competing tribes, groups, or individuals.
Those were the type of conflicts that were usually nothing more than the fair competition for territory or booty.
Now look at our enemy; we are told they are evil and come from darkness and want to destroy everything good.
They have weapons of mass destruction and want to attack the United States of America and crush us into submission.
Read full article about Best American made rifle scope.
Those are not groups of individuals running around with machetes; these are groups of organized military forces, which wish to defeat the United States of America and rule the world.
These are the group of individuals and nation-states that seek to dominate the human race with nuclear weapons.
So this is the biggest problem we face, and the only solution in my opinion; other than defeating them with the greatest armaments, is to bring in our greatest American-born minds and apply our brightest ideas into the development of these weapons.
We must create the most powerful weapons in the world, to kill off these terrorists right now.
And I intend to do this.

Because I am convinced that if we fail to do this, then the battle never ends.
Think about it; how long have we been in Afghanistan?
Twenty-seven years I believe, and that is plenty of time.
During that time the United States of America has had the most powerful military on the face of the earth.
More powerful than any other military in the entire world.
Now the Chinese have a navy with three known nuclear power plants, but do they have a fighter aircraft that can take off from China and fly to Afghanistan?
I am not saying this is fair, but I am simply stating the facts as I see them.
It is amazing how our elected officials will bend the knee before the American people and tell us that we need the largest number of military personnel ever.
Yet when it comes to sending our finest warriors to die in our wars overseas; they are only interested in the size of our Navy.
Well, I am here to tell you that is BS!
It does not matter what the size of the Navy is, what matters is how many of those ships are equipped to protect our troops.
The strongest navy is not the one with the largest number of ships, it is the one that can send the most fighters to combat.
They may have more aircraft carriers, but they are not the ones with the most powerful weapons.
Therefore, let’s get serious about fixing the problems within our military.
Do not give more resources to any politician that supports more military spending.
Please consider all this.
How to Win in a Casino?

There are so many people that want to know “How to Win in a Casino.”
This is one of the most exciting games around and it can give you the thrill of excitement.
I’m going to let you in on a little secret; if you play the game for fun, then you will most likely not have a chance of winning any money, but if you are playing to win money, then you are definitely going to have a chance of winning.
Now I have to get this out of the way, I’m not saying that if you are playing to win money, you can’t win.
That would be impossible.
However, there are certain ways to increase your chances of winning.
The first way is to do your homework before you start playing.
If you go into the casino knowing what you are doing, then you will be able to know when to walk out.
It’s a common misconception that if you bet more, you will win.
In the world of casino games, this isn’t always true.
There are certain games like Poker and Blackjack where you are taking a stand and betting your money.
These games aren’t always based on luck, although they still can’t hurt you if you have some great luck.
If you are an intelligent person then you will find a way to use the odds of the game to your advantage, source 메리트카지노.
Another tip in playing the game of chance is to know the odds.
Casino games are generally designed to be a little bit luck-based.
This is why there are so many people who think if they have the right cards or coin or something else that they will win.
Well, that’s just not true, because you are still using chance as part of the equation.
One of the best ways to keep up with the game and learn about it is to play various games.
You need to get a feel for each one and know what you need to do to win.
For example, in Poker, depending on which type of poker you are playing, you may need to hold on to your money until you see a winning hand.
However, Blackjack is a game that requires you to bet the amount of the pot and hopes you get a winning hand.
This is where you need to watch the other players and their hands because they might have the winning cards, but they also might have the amount they need to payout to leave you out of the pot.
Online gambling is another popular game for those of you who enjoy playing online games.
Most casinos offer some sort of online gambling games including online slots, video poker, blackjack, bingo, and other games.
The nice thing about these games is that you don’t have to leave your home.
You can play any time of day or night, and the money is sent to your account electronically.
Unlike live games, you can decide whether you want to wager more money or not, and you win by at least the maximum amount that you put into the pot.
If you are a new player, you may want to play a few online slots first, and learn how to play.
Then you will know when it is your time to increase your bets and when it is time to fold.
You can also decide how much to bet with each hand and decide when you are in control of the situation and ready to win or fold.
There are a number of other features that can be used, and you may want to sign up for an online casino that allows you to play multiple games, for example, keno, roulette, slots, and poker.
These online casinos typically give you a variety of bonuses as well.
One of the best ways to learn how to win in a casino?
Playing the game itself!
That is why gambling has been so popular for centuries.
The more fun you have playing the game, the more you will learn, and the more you will become successful at this exciting game.
And the best part is that with a little bit of work and knowledge, you can win a lot of money while you are having fun!
Best Cars For Beginners

The most important factor in buying a car is finding the best cars for beginners.
There are so many cars out there are thousands of websites selling cars.
With all these options to choose from, you have to take time and effort in choosing which car to buy.
There are many things that you can do to help you get started with your search quickly and easily.
Firstly, you will need to research car prices online to find out what is the average price for the model you want to buy.
In fact, this research can give you a better idea about the type of car you want.
In fact, you may not know how much you should pay initially.
This is because you will need to calculate the maintenance and gas charges into your budget.
After doing some research, decide what car you need.
What are the basic requirements of a car?
How much room do you want?
Do you plan on parking your car outside your home or inside your house?
Do you need an automatic car alarm?
Now it’s time to do some research.
You can use the Internet, your friends/relatives, newspapers, magazines, or even your friends’ cars to get the information you need.
You may also want to visit car shows to view the latest cars and check out the designs.
Then decide where you plan to buy your new car from.
Do your research.
Make sure you check how long a car lasts.
Check how reliable they are.
Read reviews online and compare prices from different stores.

Make sure to buy a car that you can afford to pay monthly or yearly.
Now you have your list of cars.
Decide which is best for you.
Remember to check the engine size, horsepower, price, and whether the car has automatic or manual transmissions.
You should also check out if the car needs new tires, batteries, or whether it will work with your existing battery.
Browse through car websites to see the latest models.
Get information about the price, model, best leisure battery, and different extras. Read customer reviews.
When you feel you have found the perfect car, make an appointment to test drive.
Test-drive a few different models and see what suits you best.
Now it’s time to buy.
Once you find the right car, research how to finance the car.
If you can’t buy the car outright, find a loan company.
You should also research and plan out how much you will spend every month on the car.
Check all the details before you finalize your deal.
You might not have to wait for a long time before you can drive the car you bought.
There are various car financing companies that you can choose from.
They offer a variety of auto loans, and you can get them approved almost immediately.

After you get your loan, always keep your car in good condition.
Regular maintenance and regular repairs can extend the life of your car.
This is very important, especially if you are buying a used car.
Ask your mechanic to give you advice on how to take care of your car.
Be careful when you buy a used car.
Before you look at any particular car, check its history and ask the seller to show you previous documents.
Most sellers will be honest, but there are some who will try to hide problems or liabilities.
If you don’t know anything about the car, ask the seller about all the technical details.
One thing you need to remember when buying cars is that it is better to buy cars that are still under factory warranty.
This way you can be sure that the car is not made to run away from you.
It is also important to get cars that come with excellent customer support services.
Look for information about service centers, warranties, registration, mileage, and other important information.
Before you buy a car, you should also check whether the car you are considering has received an excellent safety rating.
The most important thing you should do before purchasing a new or used car is to research well.
This way you will get the best possible deal on a car.
You can check with your local newspaper, the Internet, and even your friends and family to obtain more information.
Sex Tips for the Best Sex Ever!
Today, we all know that our sexuality is a gift and as such, we should treasure it.
In order to do that, we need access to great sex tips for couples.
Sex tips for couples are easy to come by.
The internet is loaded with information on everything and anything sexual.
You can get tips about sex positions and toys that will make your partner think you have been practicing for years.
We can’t deny the fact that sex is a crucial part of any relationship.
Therefore, we should take it very seriously.
If we treat it casually, it could lead to a breakup.
Sex is best left to the professionals who know what they are doing!
In addition, sex tips for couples tell us that to satisfy our partners, we need to be receptive and understanding.
This is because sex is all about being open and showing how much you enjoy giving pleasure to the person you are with.
It may be hard to believe but, one of the best sex tips for couples tells us to be a tease.
Yes, it sounds strange but, if you really look into it, you will see that this tip will have you having more fun than you thought you would.
If you are going to tease your partner, make sure you do it in such a way that your partner will be shocked.
Teasing your partner will make you feel sexy and will build a strong connection between you and your partner.
You can turn on your partner to have the best time of his or her life and, if you are good enough, they will keep coming back for more.

If you have ever seen a movie where a character is lying to his or her partner, you have a pretty good idea of what being a good tease is all about.
Good teases consist of using words like, “You look delicious tonight”, “I want to tear off your clothes” or “I can’t seem to take my eyes off you”.
You want to create an atmosphere where your partner cannot escape.
This makes him or her desire you even more.
Sex tips for couples tell us that to increase excitement, we should explore our sexual fantasies.
Sometimes, we are so caught up in our daily lives that we forget to explore our fantasies because we are so focused on living a normal life.
If you are the type of person who likes to talk dirty during sex, then make sure you let your partner know about it.
If not, you might find yourself alone wondering why your partner does not seem to find you attractive any longer.
Sex tips for couples also tell us that if we follow these tips, we will be much happier in general and, in turn, our partners will also be happier with us.
This will make sure that we are a lot happier when we are with our partner and, we hope, this will also make us feel a whole lot more aroused.
We need to let our partners know that we can do no wrong.
This does not mean that we are trying to change our partner into someone else but it does mean that we need to respect him or her and learn to love them as they are.
This might take time but, the end result will be worth it.
Best Internet Service Providers?

So, what are the best internet service, providers?
It can be quite a challenge to find one that can give you a service that is up-to-date, while still offering you the services you need and at an affordable price.
One way to differentiate yourself from your competition is to make sure you have the latest technology.
You want your service provider to have all the latest equipment and software to deliver top-notch service.
There are many options available when searching for the right internet provider for you.
Each company offers different packages and prices.
Spend some time reviewing the different providers available and then compare them based on various factors.
It’s important to look into everything from pricing, reliability, customer service, and download speeds to help ensure you choose the right option for your needs.
Here are a few things to look for to ensure you find the right company:
The speed of your internet connection is important.
There are some service providers that offer extremely fast downloads, but there are others that are almost impossible to download anything from.
Make sure you take a close look at download speeds since this is important if you need high quality with your download.
You may also consider the cost and reliability of the internet service provider.
Are you going to stick with them for a while or do you feel that they aren’t as reliable as they claim?
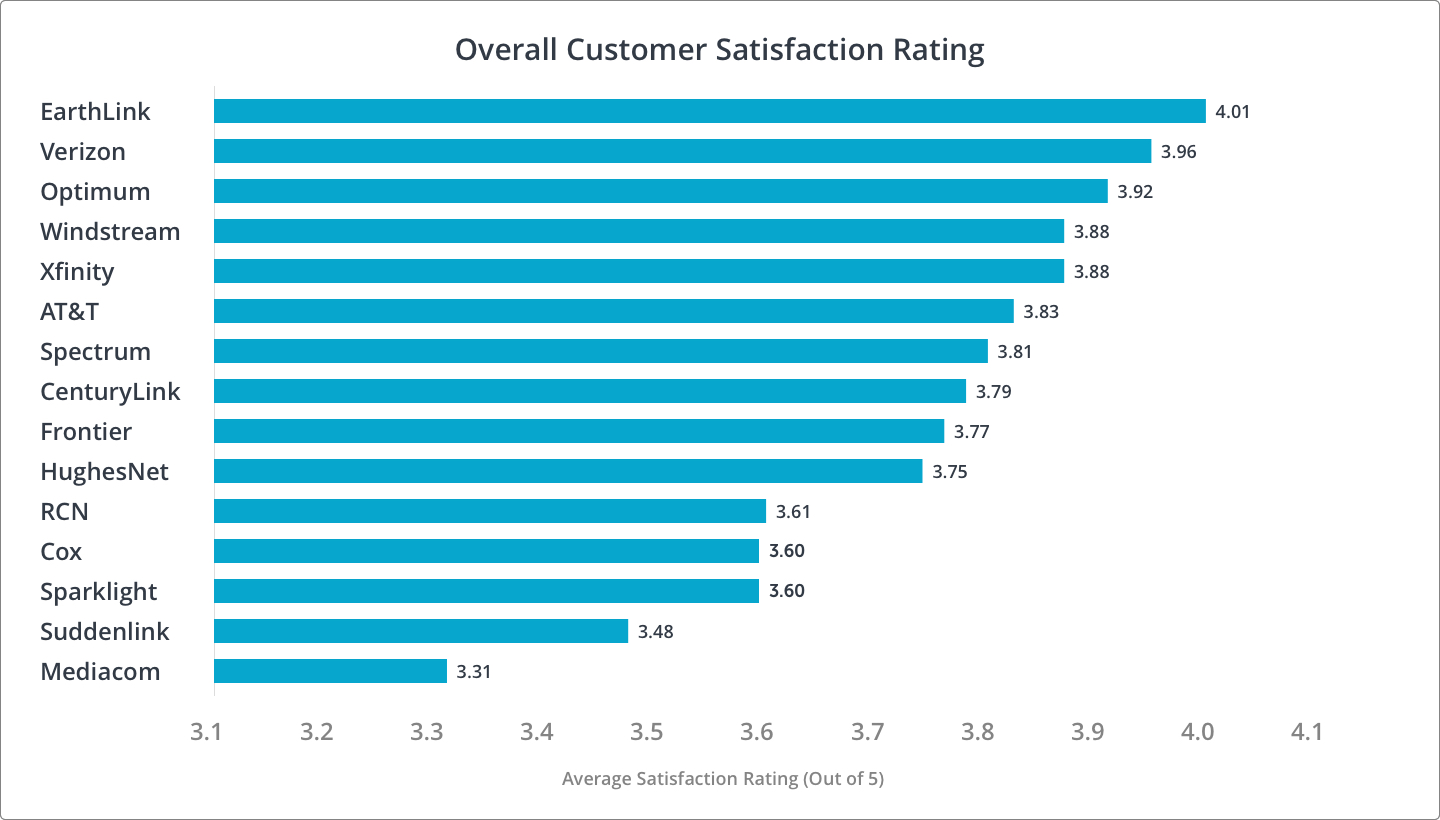
When it comes to service, you want dependability.
Not only is reliability important but you want consistent service.
If your service goes down a lot, it can seriously affect your ability to get work done and spread your ideas around the office.
Look into service providers that offer a money-back guarantee so if you aren’t satisfied, you can get your money back.
Once you’ve narrowed your search to a handful of providers, check into their customer service.
You want to work with people who are knowledgeable about the different internet plans they offer and are able to assist you with any problems or questions that you have.
Check out the online reviews and network digital signage tips of the internet companies that you are most interested in seeing what their customers have to say.
One of the worst things that can happen when choosing from the many service providers is getting a poor service plan.
You don’t want to sign up with the first company you run across, which means do your research and pick the internet service that fits your needs the best.
The more you know about the companies and the service they offer, the better off you’ll be.
Internet service providers are plentiful, so take your time, learn about each one, and choose one that offers high-quality service.
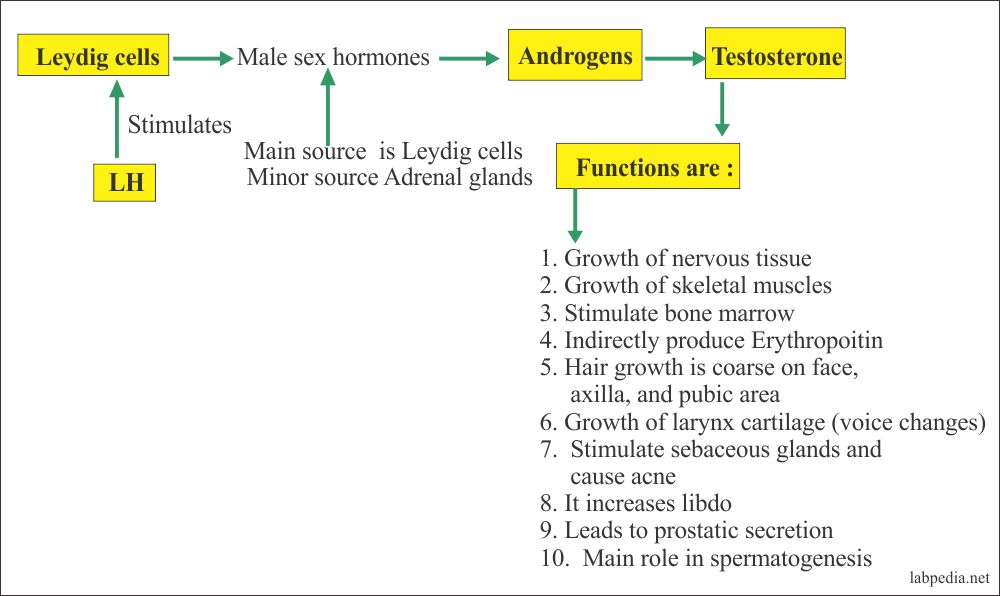
Testosterone: Functions

Testosterone is a hormone that has many important functions in the body.
First, it is an anabolic hormone, meaning it promotes the growth of bone and muscle tissue as well as serving to maintain the health of reproductive organs such as the penis and prostate.
Second, testosterone is a metabolic substance that controls other hormones such as estrogen and is key to the production of sperm.
And third, testosterone is an anabolic androgenic hormone that is responsible for maintaining bone mass and muscle mass and is critical in the recovery and repair of muscle tissue after physical injury.
As you can see, there are many different functions that testosterone plays in the body.
It is vital for men to produce and maintain high levels of testosterone, which is why men are at a greater risk of developing…
- Androgynous sexual disorders
- Low sperm counts
- Decreased production of muscle
- Bone Tissue
- Decreased muscle and bone strength
- And decreased libido.
Testosterone deficiencies can have a devastating effect on a man’s sex and reproductive health.
To compensate for these deficiencies, men have developed products to artificially boost testosterone in the body.
However, while these supplements may help a man to some extent, they do not address many of the deficiencies.
Most of the testosterone deficiencies are caused by the low bioavailability of testosterone.
Low bio-availability means that the testosterone gets eliminated from the body before it can perform its functions.
This means that the body must rely on external sources for the production and release of testosterone, and this can be very difficult.
Some supplements may help to improve the body’s bioavailability of testosterone, but they also contain contaminants that can further compromise the body’s bioavailability of testosterone.
Some supplements may include artificial ingredients and chemicals, synthetic hormones, and other chemical contaminants that can interfere with the production and release of testosterone.
Another way that testosterone supplements can interfere with the androgenic properties of the body is through their use in men who have hypogonadism.
This means that the body produces too much testosterone or lacks the ability to produce testosterone at all.
These supplements may temporarily increase the testosterone levels of a hypogonadism patient, but once the effects of the medication wear off, these levels will usually decrease again – https://steroideapotheke.com/roidstation-com-alternative-2020/.
This can be frustrating for a person trying to treat his or her condition with testosterone deficiency and can also lead to harmful side effects.
A third way that testosterone supplements can interfere with the body’s ability to naturally balance testosterone production and release is through their use in a person suffering from Andropause.
As men go through the process of aging, the amount of testosterone produced and stored in the body gradually decreases.
Testosterone deficiency symptoms in older men are usually depression, decreased sex drive, loss of muscle mass, decreased energy levels, and hot flashes.
While testosterone replacement therapy can sometimes help relieve these symptoms of Andropause, these supplements can actually stimulate the production of testosterone and thus increase these symptoms even more.
There are some drawbacks to taking testosterone supplementation.
Most notably, because testosterone is an anabolic hormone, it requires an anabolic environment to be released and does not easily fit into a diet or lifestyle.
For this reason, it is much more commonly used as a dietary supplement than a topical one.
Moreover, testosterone is made by the liver, so any problems with this organ could lead to other serious health issues.
While there are many benefits to testosterone, its use should be carefully considered and used as directed.
Natural Breast Health

Natural Breast Health – Preventative and traditional Chinese medicine
Some call it “bottle preference”.
Or “self-weaning”.
But when it happens suddenly and definitively, without the participating intention of Mom, it feels a bit like rejection.
I’m talking about the moment when your baby decides on his own that he’s done with sucking on mom to get milk.
“Why should I work so hard and have to wait almost a *whole minute* for the letdown response to happen when there’s a bottle option that is way easier and instantaneous?
Get this boob out of my face, mommy!
And bring me a bottle!
Quickly now, I will just lie here wriggling and crying until you return.”
Nursing had always been my go-to Universal Remote Codes.
My sure-to-work baby calming tool.
I had earned this ultimate mommy negotiating technique after months of inflamed milk ducts and raw, lanolin saturated nipples.
Hadn’t I?
Why had it suddenly stopped working?
Flashback to a couple of days after Tor was born.

I hand-pumped when Tor was asleep to help get my milk to flow, and I was pretty happy about the half-ounce of milk I had been able to collect.
As we were about to feed that milk back to Tor in a bottle, our midwife knocked on the door for a post-partum house call.
When she saw what we were doing, she first congratulated me on my new milk.
And then with a calm urgency, she recommended we encourage Tor to only drink from me until my milk was well established.
She alluded to this idea of “nipple rejection”, where babies can learn that bottles take less effort to drink from than breasts do.
And if that happens, and you still want your baby to enjoy all of the benefits of breast milk, then your options are pumping several times per day or using a milk bank.
I knew I wanted Tor to be exclusively fed breast milk for his first 6 months and hopefully for longer, so 2 days post-partum we stopped using a bottle altogether.
That is until it came time for me to go back to work when he was about 9 months old.
For a few weeks before that, we trained Tor to take a bottle every once in a while since he was going to have to use one when I wasn’t here.
And then came a day came I left Tor and his Dad at home for the afternoon while I went out shopping.

Tor happily drank from the bottles he was offered while I was gone.
I didn’t know at the time that when I nursed him to sleep that night, it would be for the last time.
When he woke at 11 pm for his usual first feed of the night, he was upset and inconsolable.
After a period of fussing and getting genuinely angry when I would try to get him to latch, he accepted a bottle, rolled over, and fell asleep.
And although I offered to nurse him every time he fed for the next several weeks, a bottle is the only way he drinks milk anymore.
It happened in one instant.
I see the positive in this – I didn’t have to wean him, pumping can be a lot more time-efficient and bottles are somewhat easier than breastfeeding when you’re on the go (and the only option when driving).
Plus, the biggest bonus has been that dad can now feed Tor during the night so mom can put her earplugs in and sleep for 6-8 hours straight until her boobs are so full they wake her up.
It’s just too bad that pumping is so much more physically painful compared to nursing.
(I still sometimes miss that unbelievably intimate bond of breastfeeding.
Holding a sleeping, satiated, flutter sucking baby is pretty sweet…).
Good Oral Health is more than white teeth and a pretty smile

In the United States, one person every hour of every day dies of oral cancer.
In women, its rate is higher than the rate of cervical cancer, and it is the sixth leading form of cancer among men.
An alarming 25% of victims have no lifestyle risk factors for the development of oral cancer, and it is being diagnosed at an increasing rate among young adults.
There is a high survival rate among sufferers when detected early, but in its late-stage, the five-year survival rate is a modest 57%.
Oral cancer does not discriminate and most people are not even aware that they are at risk.
Scientists have recently established a connection between experiencing an HPV viral infection in the mouth and this type of cancer.
Additional risk factors are:
- Tobacco and Alcohol use
- Men between the ages of 40 and 60
- A family history of oral, head, or neck cancers
- Poor oral hygiene, including the irritation of oral membranes caused by rough surfaces and broken or protruding teeth
- Poor nutrition
There are many types of oral cancer, but the vast majority may start in any tissues that line the mouth or lips. Advanced stage symptoms might include a lesion, lump, or ulcer on the tongue, lips, or mouth that does not heal within two weeks.
An individual may also experience difficulty in swallowing, white or red patches in the mouth, and pain, tingling or burning of the oral cavity.
Unfortunately, in its late stage, oral cancer treatment options are limited to surgical removal of the affected tissue, and subsequent reconstructive surgery to correct disfigurement, which can result in the limited ability to swallow, high-frequency hearing loss, and sinus damage.
Fortunately, advancements in technology have unveiled a powerful tool for assisting in the discovery of oral cancer at its earliest stage before it can even be detected by traditional visual oral exams!
Since the Fall of 2010, our dental office has been one of the few practices to include the VELscope Vx oral cancer screening as part of our patients’ comprehensive oral exams.
This cutting edge technology utilizes a narrow band of safe, high energy blue light with special filtering characteristics to thoroughly evaluate oral tissue for cancerous lesions that escape the naked eye.
A recent study conducted by the University of Montreal concluded that the inclusion of the use of this screener in comprehensive oral exams significantly increases the detection rate of oral cancer in its earliest stage when its survival rate is at least 90%.
At the office of Dr. Carrie Hansen, DDS, we care about your health as well as your teeth.
By including the use of the Velscope Vx cancer screening technology as part of our patients’ oral exams, we have reaffirmed our proactive approach to oral care by detecting abnormalities when proper treatment can have promising results.
Swedish testosteron tillskott

You’ve probably heard of the hormone testosterone. The more natural testosterone you have, the greater the increase in muscle mass etc. An easy way to naturally increase the amount of testosterone in your body is through a testosterone enhancing supplements. Important to know the difference between testobooster and synthetic testosterone, which is illegal. A swedish “testosteron tillskott” has the goal to raise your levels to those natural, but synthetic has the aim to raise your levels to over them natural.
What is so called testosteron tillskott?
Testosterone is a hormone that promotes muscle growth. As the sound of the name is a testobooster (testosteron tillskott) a supplement that will increase the amount of testosterone naturally. The more natural testosterone, the greater the increase in muscle mass for hard-training individuals. More information about the so called ”swedish naturligt testosteron tillskott” can be found here.
How does a swedish testosterontillskott work?
Only buy a product that is 100% legal and natural. NOTE: You should buy from well-known brands, Swedish testosteron tillskott is preferable. This is because it has happened several times that rogue businesses mixed in illegal substances in their testoboosters for people to like them extra.
A testosterontillskott works by combining several ingredients that increase testosterone in the body. Because there are many subjects in scientific studies to increase the natural testosterone. Some have much and “heavy” research behind them, while others are more recently discovered and only preliminary results. Some of the substances have been shown to affect testosterone in the body and is usually included in a testosterone booster is as follows:
- Zinc
- Magnesium
- D-Vitamin
- Tribulus Terrestris
- DAA
- Macaextrakt
- Onions and garlic extract?
Dietary supplement
If you look a little closer at the contents of a testobooster you can draw your own conclusions if you think it’s working or not. Among other vitamins and minerals are said to be able to raise testosteron levels naturally. When you combine these substances in one tablet can increase testosteron levels naturally. But if you already have extremely high levels through optimal nutrition as a “testosteron tillskott” not make much difference. But there are very few that come up in these levels through diet alone.
What do avoid!
It is not unusual that the criticism directed at testoboosters often as it would raise the testosterone levels in the same way as anabolic steroids (synthetic testosterone). However, the purpose of a testobooster not raise your testosterone levels to those of the natural, but just to raise your levels to those natural.
Some Summarizing words of testosteron tillskott
Please just try a swedish naturligt testosteron tillskott to increase your levels. However, one should realize that they do not make you a “Belgian Blue” and muscles swell up overnight. A testobooster serves as said by maximizing your natural levels. Had the increased levels of the natural had been illegal . It really is not. But when you work seriously so is every extra% you can get gold worth. Therefore, a booster may not be recommended for a semi-serious hobby trainer, but it is something you really want to get good results! Then, one should not forget the psychological impact of a Testo booster either.
Who Should Get Doctor at Home Visit Services In Dubai?

Dubai is well regarded for offering world-class medical services and health services like doctors on call Dubai. It is not easy to take care of your health in this day to day life. Being sick is one of the most stressful parts of life, especially when you need to visit the hospital too frequently. At this time, you feel hopeless and wish to improve your health fast. This is why we need home visit doctors Dubai for ample convenience.
Services Offered
Home healthcare providers offer a lot of services like primary care which includes treatment, diagnosis and care for the people with several health issues. Primary healthcare providers help monitor and manage pre-existing and ongoing conditions.
These doctors also provide vitamin injection Dubai to avoid diseases and maintain overall health. They provide services with vast experience and knowledge. They also perform routine checkups to keep track of your health and ensure your positive response to treatment. They also offer speech and physical therapies. These services are beneficial to the people of all ages, especially the ones who are unable to travel to hospitals and those who need special care.
What to Expect with Doctors on Call?
There are many benefits of doctors on call for residents of Dubai. Here’s what you can expect from home healthcare service providers –
Availability
We often worry a lot, especially when our loved one is sick or we have a child at home, and we are away from them. This way, home healthcare service providers can ease the burden by being around. We can also make changes to their services. You may not be able to go anywhere when you are sick, or you might not have the proper strength to reach the clinic. This way, calling the doctors is as simple as requesting and dialling services from an expert physician. It can also be made simple with portable medical tools to get the best services.
Family Help
In hospitals, you can only visit your loved one for specific hours. But if you have a doctor on call, you can always remain at home where your friends and family can visit all the time. There is also no need to worry about an unknown environment or a standard room to share with other patients. It also improves positive response to medication and therapy and faster recovery.
Reduces hospital readmission
By investing in in-home healthcare, you can significantly reduce the odds of getting readmission in the hospital. This way, there are high chances of recovery and lower chances of hospitalization. There are also reduced risk of getting infections, which take place after a long inactivity period, especially when you are taking bed rest which can slow the recovery time at the hospital. This way, home healthcare facilities can speed up recovery in a cosy environment.
Better Care
Home healthcare providers treat patients at their own pace without being in a hurry. There is also no queue of patients who are waiting to see their doctors. When a doctor visits your home, he can take a proper test and address your concerns personally. They can work on your case without any interruptions. You are the only patient they need to serve.
Cost-Effective
In comparison to getting admitted into a hospital, a doctor on call service is quite less expensive. They provide all the facilities to people who are released from the hospital but need specialized care. You can also save on consultation charges and get the same services as you get in hospital.
Bottom Line
All in all, home healthcare facilities are very beneficial for the people of all ages, especially young children and the elderly. It can save on doctors’ fees and hospitalization. It also helps avoid infection due to hospital stays.
Author Bio
 I am a Health Writer and usually checks health treatment country wise, state-wise and city-wise. I found Dubai is best for health treatment. One can get Doctors on-call Dubai.
I am a Health Writer and usually checks health treatment country wise, state-wise and city-wise. I found Dubai is best for health treatment. One can get Doctors on-call Dubai.
